AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Office outpatient visit9/2/2023  In an office or outpatient setting, another consultation may be requested of the same consultant practitioner if the consultant has not been providing ongoing management of the patient for this condition after his/her initial consultation. Kane…”Įvaluation : “Dear Jim, thanks for asking me to evaluate Betsy for…” Hoff for my advice about…”Ĭonsult : “Patient seen in consultation at the request of Dr. Request : “Mr Jones is seen in consultation at the request of Dr Kane for evaluation for abdominal pain…"Īdvice : “Patient sent by Dr. Your documentation should state the request, name of the provider requesting the consultation, and the reason for the consultation.Įxamples of appropriate documentation are: The statement “Thank you for referring” is not enough documentation to support the request. The written request and reason for a consultation must be included in the consulting practitioner’s plan of care. 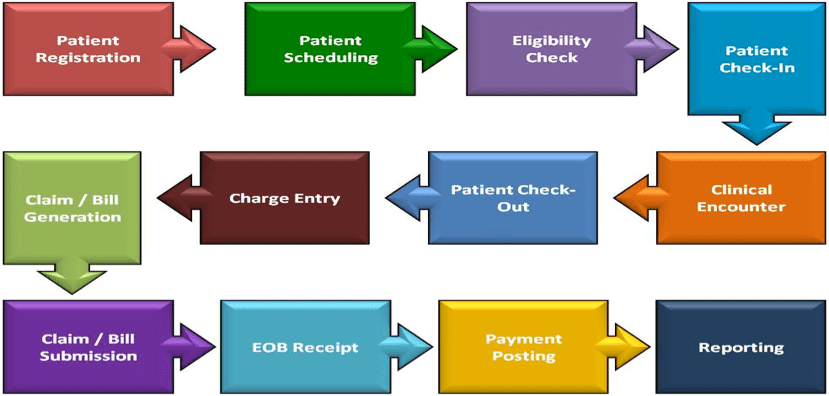
A written request and reason for a consultation must be included in the requesting practitioner’s plan of care. Enter the selected code in the box above.Ĭonsultation services require 3 things: (i) a request from an appropriate source (ii) the consultation evaluation service and, (iii) a written report. If the new patient visit CPT codes are not on your Epic speed buttons, you must go to the Charge Capture screen in the Visit Navigator and click in the "None" hyperlink found in the Additional E/M Codes box o locate CPT codes 99201-99205. A "new patient" is a patient who has not received any professional services, i.e., evaluation and management service or other face-to-face service (e.g., surgical procedure) from the physician or physician group practice (same physician specialty) within the previous three years. However, performing two services but charging for only one isn’t reasonable for practice revenue and doesn’t follow CPT rules.The limitation of ten speed buttons in Epic Ambulatory has sometimes caused confusion with billing the new patient visit codes or a consultation. Note that neither CPT nor CMS requires a change in treatment to support billing for a second separate service.įamily physicians are sometimes reluctant to add this second service because they know the patient will be charged a copay or, depending on the deductible, the full fee for the problem-oriented visit. This could include ordering or reviewing diagnostic tests, renewing prescriptions, making referrals, or implementing other changes to treatment. In your documentation, you should describe in the history of the present illness all of the patient’s acute or chronic conditions and should detail in the assessment and plan how you managed them, making sure to show your extra cognitive work. 
“That portion of the visit must be medically necessary to treat the beneficiary’s illness or injury, or to improve the functioning of a malformed body member,” says CMS. Likewise, the Center for Medicare & Medicaid Service’s (CMS) guide to wellness visits states that when you furnish a significant, separately identifiable, medically necessary E/M service with a wellness visit, add the E/M service with modifier 25. Here’s some quick guidance from CPT: If a new or existing problem is addressed at the time of a preventive service and is significant enough to require additional work to perform the key components of a problem-oriented evaluation and management (E/M) service, you should bill for both services with modifier 25 attached to the latter. 
How do you quickly determine if you should add a second service and bill for a separate problem-oriented visit? In other words, when should you bill an office/outpatient service (CPT codes 99212-99215) on the same day as a preventive medicine service (CPT codes 99381-99397) or a Medicare wellness visit (HCPCS codes G0402, G0438, or G0439)? Let’s say a patient comes in for a preventive medicine service and you end up also treating an acute or chronic problem. 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
